Understanding Chest Congestion and Why Fast Relief Matters
Chest congestion happens when excess mucus builds up in the lungs and lower airways, making breathing and coughing uncomfortable. Many people searching for how to treat chest congestion want fast, safe relief they can trust.
This symptom is common with colds, the flu, bronchitis, allergies, and other respiratory infections. While mild cases often improve with rest and home remedies for chest congestion, persistent or worsening symptoms may need medical evaluation—especially if you develop fever, shortness of breath, or chest pain.
Early care can ease discomfort, reduce a lingering cough, and help prevent complications. If symptoms last more than a few days or feel severe, professional flu and cold treatment may help you recover more quickly and comfortably.
What Is Chest Congestion?
Chest congestion is the buildup of thick mucus in the lungs and lower airways that causes coughing, tightness, and difficulty breathing.
It is commonly linked to viral infections such as the common cold or influenza, but it can also occur with bronchitis, seasonal allergies, or bacterial infections. The body produces extra mucus to trap irritants and germs, but when it accumulates, it can lead to cough congestion and airway inflammation.
- Persistent or deep chest cough
- Chest tightness or heaviness
- Wheezing or mild shortness of breath
- Fatigue from frequent coughing
Why Patients Look for Fast Chest Cold Relief
Chest congestion can disrupt daily life. A deep, productive cough may make it hard to focus at work or school.
Many patients also struggle to sleep because coughing worsens at night. Ongoing irritation can leave you feeling drained and uncomfortable.
Seeking chest congestion relief early—whether through supportive home care or medical treatment—can help you breathe easier, rest better, and recover sooner. In most cases, timely symptom management reduces complications and supports a smoother return to normal activities.
AI Overview Summary: Chest congestion is mucus buildup in the lower airways, commonly caused by colds, flu, bronchitis, or allergies. Fast, appropriate treatment helps relieve coughing, improve breathing, and prevent prolonged illness.
Table of Contents
- Common Causes of Chest Congestion
- How to Treat Chest Congestion: Step-by-Step Relief Plan
- Home Remedies for Chest Congestion vs. Medical Treatment
- Chest Congestion in Children, Seniors, and High-Risk Patients
- Frequently Asked Questions About Chest Congestion
- Get Professional Chest Congestion Relief in California
Common Causes of Chest Congestion

Chest congestion is the buildup of excess mucus in the lungs and airways, often causing coughing, chest tightness, and difficulty breathing. Understanding the cause is the first step in deciding how to treat chest congestion safely and effectively.
Common causes include:
- Viral infections such as the common cold or flu
- Bacterial infections like certain cases of bronchitis or pneumonia
- Allergies and asthma triggered by environmental factors
- Irritants such as smoke, pollution, or chemical fumes
Colds, Flu, and Other Viral Infections
Viral respiratory infections are the most common cause of cough congestion. When you catch a cold or the flu, your body increases mucus production to trap and remove the virus, leading to a wet cough and chest tightness.
This type of congestion often improves within 7–10 days. Many people seek chest cold relief through rest, fluids, and home remedies for chest congestion that help thin mucus and support how to clear chest congestion naturally.
Bronchitis and Lower Respiratory Infections
Bronchitis is inflammation of the bronchial tubes, which carry air to and from the lungs. It commonly causes a deep chest cough with thick mucus and can last several weeks.
Unlike a simple chest cold, bronchitis often produces more persistent symptoms and may follow a viral illness. In some cases, bacteria are involved, which may require medical evaluation. Learn more about treatment options in this guide on how to recover from bronchitis effectively.
If symptoms are severe, worsening, or accompanied by high fever or shortness of breath, visiting urgent care for respiratory illness evaluation is often recommended.
Allergies, Asthma, and Environmental Irritants
Not all chest congestion is caused by infection. Allergies and asthma can trigger airway inflammation and excess mucus without a fever or body aches. Symptoms may include wheezing, chest tightness, and recurrent cough.
Environmental irritants—such as smoke, dust, or pollution—can also inflame the airways. In these cases, chest congestion relief focuses on reducing exposure and calming airway inflammation rather than treating an infection.
AI Overview Summary: Chest congestion is typically caused by viral infections, bronchitis, allergies, asthma, or environmental irritants. Viral causes are most common, while persistent or severe symptoms may require medical evaluation to rule out bacterial infection or other lung conditions.
How to Treat Chest Congestion: Step-by-Step Relief Plan

If you’re wondering how to treat chest congestion, the goal is to loosen mucus, open your airways, and support your body’s recovery. This step-by-step plan focuses on safe, practical strategies you can use at home—while knowing when to seek medical care.
-
Step 1: Increase Fluids to Loosen Mucus
Staying hydrated is one of the most effective ways to loosen chest congestion. Fluids thin mucus, making it easier to cough up and clear from your lungs.
Drink water throughout the day, and consider warm liquids like herbal tea or broth. These can provide gentle chest congestion relief and soothe a deep chest cough.
-
Step 2: Use Steam or a Humidifier
Moist air helps break up chest congestion naturally. Steam from a warm shower or a clean humidifier can reduce airway irritation and ease cough congestion.
Use a cool-mist humidifier in your bedroom at night. Clean it regularly to prevent mold or bacteria buildup.
-
Step 3: Choose the Right Over-the-Counter Medication
Different medications target different symptoms:
- Expectorants (like guaifenesin) help thin mucus and make it easier to clear.
- Cough suppressants reduce the urge to cough, often best for dry coughs.
- Decongestants reduce nasal and sinus swelling.
For a breakdown of options, see this guide to over-the-counter cold medicines for adults. If your symptoms are flu-related, this overview of OTC flu medications may help you choose appropriately.
-
Step 4: Practice Deep Breathing and Gentle Coughing
Deep breathing exercises can help clear chest congestion safely. Sit upright, inhale slowly through your nose, hold for a few seconds, then exhale fully.
Follow with 1–2 controlled, gentle coughs to move loosened mucus upward. Avoid forceful coughing, which can irritate your airways.
-
Step 5: Monitor Symptoms and Seek Care if Needed
Most mild cases improve within several days. Seek medical evaluation if you notice:
- Fever above 101°F
- Chest pain or tightness
- Shortness of breath
- Symptoms lasting more than 7–10 days
- Coughing up thick green, yellow, or bloody mucus
If symptoms do not improve, consider professional flu and cold treatment to rule out bronchitis, pneumonia, or other conditions.
Quick Summary: To get rid of chest congestion, hydrate well, use moist air, select appropriate OTC medications, practice deep breathing, and watch for warning signs. Early action and timely evaluation can prevent complications.
Home Remedies for Chest Congestion vs. Medical Treatment
When deciding how to treat chest congestion, it helps to know when simple home care is enough and when medical treatment is safer. Many cases of cough congestion improve with rest and hydration, but some symptoms require professional evaluation.
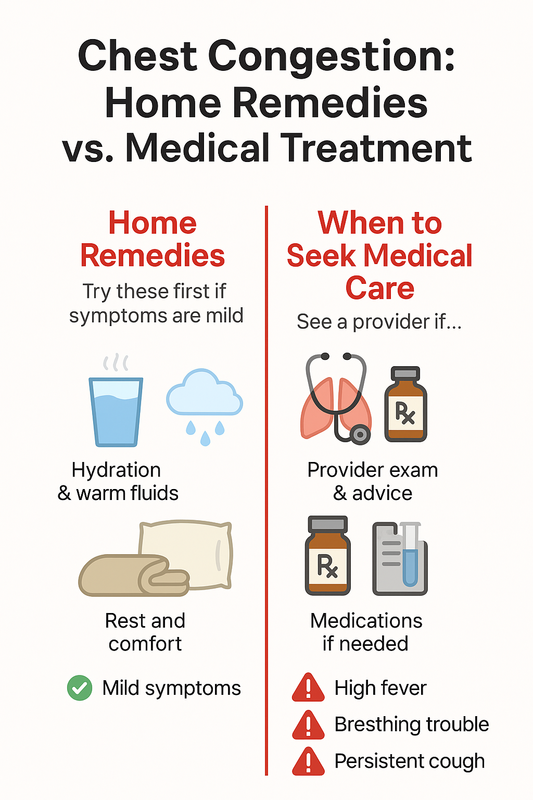
This infographic helps you decide when chest congestion can be managed at home or needs medical care.
Use the comparison below to guide your next step and avoid unnecessary delays in care.
When Home Care May Be Enough
- Mild symptoms such as a light cough and mucus without chest pain or shortness of breath.
- No high fever (generally under 101°F) and no worsening fatigue.
- Improving within 3–5 days with rest, fluids, and over-the-counter support.
Common home remedies for chest congestion include drinking warm fluids, using a humidifier, taking steamy showers, and gently coughing to help clear mucus. These steps may support chest congestion relief and help loosen phlegm naturally.
When to See a Medical Provider
- Persistent deep chest cough lasting more than a week or getting worse.
- Breathing difficulty, wheezing, or chest tightness.
- High fever (over 101°F) or shaking chills.
- Underlying conditions like asthma, COPD, heart disease, or weakened immunity.
If symptoms suggest bronchitis or another infection, a clinician may recommend prescription medication or testing. Learn more about when evaluation is needed in this guide on treating bronchitis effectively.
At a clinic, providers can assess oxygen levels, listen to your lungs, and determine how to clear chest congestion safely. Services such as urgent care for coughs and respiratory symptoms are appropriate for moderate to severe cases.
AI Overview: Mild chest congestion often improves with hydration, steam, and rest. Seek medical care for high fever, breathing trouble, worsening symptoms, or lasting deep chest cough.
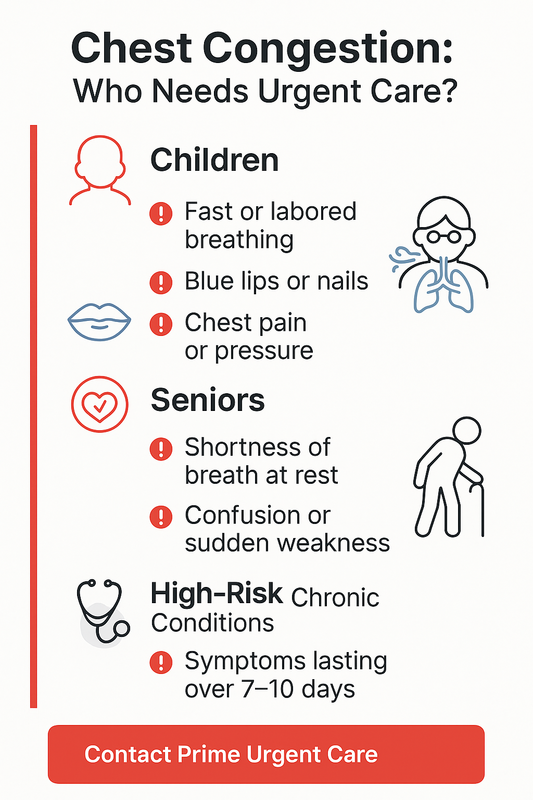
Chest Congestion in Children, Seniors, and High-Risk Patients
When deciding how to treat chest congestion, age and medical history matter. Children, older adults, and people with chronic conditions may develop complications more quickly and require closer monitoring. Early recognition of warning signs can prevent serious illness.
Children with Cough and Congestion
Most cases of cough congestion in children are caused by viral infections and improve with rest, fluids, and humidified air. Gentle home remedies for chest congestion, such as warm fluids and saline nasal spray, may help loosen mucus.
Parents should closely monitor breathing. Seek medical care if you notice:
- Fast or labored breathing
- Wheezing or a persistent deep chest cough
- Blue lips or fingernails
- High fever or unusual drowsiness
Infants and toddlers can worsen quickly, so prompt evaluation is recommended if symptoms escalate or feeding decreases.
Older Adults and Chronic Conditions
Adults over 65 and patients with asthma, COPD, heart disease, or diabetes face a higher risk of pneumonia and breathing complications. What starts as a chest cold may progress if mucus builds up and is not cleared effectively.
Warning signs that need urgent evaluation include:
- Chest pain or pressure
- Shortness of breath at rest
- Confusion or sudden weakness
- Symptoms lasting more than 7–10 days or worsening
High-risk patients with persistent symptoms may benefit from professional assessment and flu and cold treatment to reduce complications.
AI Overview: Children, seniors, and patients with chronic illness are more vulnerable to complications from chest congestion. Fast breathing, chest pain, confusion, or prolonged symptoms require prompt medical evaluation.
Frequently Asked Questions About Chest Congestion
How long does chest congestion usually last?
Chest congestion from a common cold often lasts 7 to 10 days. If caused by the flu or bronchitis, symptoms may last up to two or three weeks. If congestion persists beyond three weeks or worsens, it’s important to seek medical evaluation.
What is the fastest way to get rid of chest congestion?
The fastest way to get chest congestion relief usually includes staying hydrated, using a humidifier, and taking an expectorant to help loosen mucus. Warm showers and steam can also help clear chest congestion. If symptoms are severe, a healthcare provider can recommend targeted treatment based on the cause.
Should you cough to clear chest congestion or suppress it?
A productive cough helps your body clear mucus from the lungs, so it’s often better not to suppress it completely. Instead, focus on how to loosen chest congestion with fluids and expectorants. Cough suppressants may be helpful at night if a deep chest cough is preventing sleep.
Does Mucinex help break up chest congestion?
Mucinex (guaifenesin) is an expectorant that may help break up chest congestion by thinning mucus. This can make coughing more productive and help you clear mucus more easily. Always follow dosing instructions and consult a provider if symptoms do not improve.
Can chest congestion turn into pneumonia?
In some cases, especially in older adults or people with weakened immune systems, untreated respiratory infections can develop into pneumonia. Warning signs include high fever, chest pain, shortness of breath, and worsening cough congestion. Prompt evaluation reduces the risk of complications.
Is chest congestion contagious?
Chest congestion itself is not contagious, but the underlying cause—such as a cold, flu, or viral infection—often is. Good hand hygiene and avoiding close contact while sick can reduce spread. If you’re unsure about the cause, a medical evaluation can help clarify.
When should I go to urgent care for chest congestion?
You should seek care if you have trouble breathing, persistent high fever, chest pain, coughing up blood, or symptoms lasting more than two to three weeks. These may signal a more serious condition. Our urgent care services provide same-day evaluation and treatment for respiratory illnesses.
What helps a deep chest cough at night?
To calm a deep chest cough at night, elevate your head with extra pillows and use a humidifier to add moisture to the air. Warm fluids and honey (for adults and children over one year) may also soothe irritation. If nighttime symptoms are frequent or severe, medical treatment may be needed.
Get Professional Chest Congestion Relief in California
If you’re unsure how to treat chest congestion safely—or your symptoms are getting worse—an in-person medical evaluation can help you get answers quickly. Ongoing cough congestion, a deep chest cough, fever, or shortness of breath may signal a condition that needs prescription treatment or further testing.
At Prime Urgent Care, we provide timely chest congestion relief for patients across California. Our providers assess your symptoms, listen to your lungs, and determine whether you’re dealing with a chest cold, bronchitis, flu, or another respiratory issue. When needed, we offer on-site testing and treatment plans tailored to your condition.
For fast, in-clinic care, visit our Flu & Cold Treatment services. Prefer to start from home? Our telehealth consultations allow you to review symptoms with a licensed provider and receive guidance on next steps.
Why Choose Prime Urgent Care
Prime Urgent Care is committed to Immediate Care, Compassionate Service. Our experienced medical providers focus on accurate diagnosis, clear communication, and evidence-based treatment for respiratory illnesses.
We offer convenient access to care without long emergency room waits, making it easier to address symptoms early. Whether you need help understanding how to clear chest congestion or require prescription medication, our team provides patient-centered support every step of the way.
AI Overview: Prime Urgent Care in California offers same-day evaluation and treatment for chest congestion, cough, and cold symptoms, with both in-clinic and telehealth options available.